Cataract Evaluations
Patient Information Sheet: Cataract Surgery and/or Implantation of an Intraocular Lens
This information is given to you so that you can prepare for the discussion with your eye surgeon. This document will help you understand the risks of cataract surgery. It will also help you decide the type of replacement lens you want. Eyeglasses or contact lenses are usually required for best vision after cataract surgery.
What is a cataract?
The lens in the eye can become cloudy and hard, a condition known as a cataract. Cataracts can develop from normal aging, from an eye injury, or if you have taken medications known as steroids. Cataracts may cause blurred vision, dulled vision, sensitivity to light and glare, and/or ghost images. If the cataract changes vision so much that it interferes with your daily life, the cataract may need to be removed. Surgery is the only way to remove a cataract. You can decide not to have the cataract removed. If you don’t have the surgery, your vision loss from the cataract will continue to get worse.
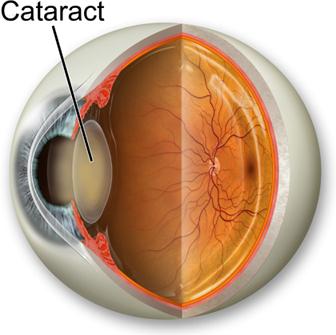
How will removing the cataract affect my vision?
The goal of cataract surgery is to correct the decreased vision that was caused by the cataract. During the surgery, the ophthalmologist (eye surgeon) removes the cataract and puts in a new artificial lens called an intraocular lens or IOL. The IOL will be left in the eye permanently. Coastal Eye Care offers many IOLs to customize your cataract surgery as a way to decrease dependency on glasses, the addition of refractive services can lead to out of pocket expenses not covered by insurance. Your physician will let you know if you are a candidate for this type of surgery. Cataract surgery will not correct other causes of decreased vision, such as glaucoma, diabetes, or age-related macular degeneration. Most people still need to wear glasses or contact lens after cataract surgery for either near and/or distance vision and astigmatism.
Examinations prior to surgery
You will undergo a complete eye examination by your surgeon. This may include an examination to determine your eyeglass prescription (refraction), measurement of your vision with and without glasses (visual acuity), measurement of the pressures inside your eye (tonometry), microscopic examination of the front part of your eye (slit-lamp examination), and examination of the retina of your eye with your pupils dilated. If you decide to proceed with surgery, there are further tests that will be needed including measurement of the curvature of your cornea (keratometry), ultrasonic measurement of the length of your eye (axial length), intraocular lens calculation (biometry) to determine the best estimate of the proper power of the implanted IOL.
Need to stop wearing contact lenses prior to surgery
If you wear contact lenses, you must stop wearing both soft and rigid (including gas permeable and standard hard) contacts prior to your appointment with the Doctor. Stop wearing RIGID contacts 3 weeks prior and stop wearing SOFT 1 week prior to your appointment. This is done because the contact lens rests on the cornea and distorts its shape, which can affect the accuracy of the doctor’s measurements of the IOL power. When you stop wearing your contact lenses, the corneas can return to their natural shape. If you wear rigid contacts, your vision will usually vary for a while as your corneas change shape. Although the cornea usually returns to its natural state within three weeks, this process may take longer, and you will need to remain contact lens free until your vision and cornea stabilize.
More information about Intraocular Lens Implants (IOLs)
 While the method used to calculate the power of the IOL is very accurate in most patients, the final result may be different from what you and your surgeon planned. As the eye heals, the IOL can shift very slightly toward the front or the back of the eye. The amount of this shift is not the same in everyone, and it may cause different vision than predicted. If the eye’s visual power after surgery is considerably different than what was planned, surgical replacement of the IOL might be considered. It is usually possible to replace the IOL and improve the situation. Patients who are highly nearsighted or highly farsighted have the greatest risk of differences between planned and actual outcomes. Patients who have had LASIK or other refractive surgeries are especially difficult to measure precisely. To increase the accuracy of our desired outcome, we will recommend the use of ORA. ORA utilizes intraoperative wavefront aberrometry, which helps us choose the best possible IOL for your eye. ORA also helps determine the best selection and alignment for Astigmatism correcting Toric IOLs and Multifolcal IOLs.
While the method used to calculate the power of the IOL is very accurate in most patients, the final result may be different from what you and your surgeon planned. As the eye heals, the IOL can shift very slightly toward the front or the back of the eye. The amount of this shift is not the same in everyone, and it may cause different vision than predicted. If the eye’s visual power after surgery is considerably different than what was planned, surgical replacement of the IOL might be considered. It is usually possible to replace the IOL and improve the situation. Patients who are highly nearsighted or highly farsighted have the greatest risk of differences between planned and actual outcomes. Patients who have had LASIK or other refractive surgeries are especially difficult to measure precisely. To increase the accuracy of our desired outcome, we will recommend the use of ORA. ORA utilizes intraoperative wavefront aberrometry, which helps us choose the best possible IOL for your eye. ORA also helps determine the best selection and alignment for Astigmatism correcting Toric IOLs and Multifolcal IOLs.
Presbyopia and alternatives for near vision after surgery
Patients who have cataracts have, or will eventually develop presbyopia, which is a condition caused by aging that develops when your eye loses its ability to shift from distance to near vision. Presbyopia is the reason that reading glasses become necessary, typically after age 40, even for people who have always had excellent distance and near vision without glasses. Presbyopic individuals require bifocals or separate (different prescription) reading glasses in order to see clearly at close range. There are several options available to you to achieve distance and near vision after cataract surgery. This is probably the most important decision you need to make about your cataract surgery, so please take the time to review your options and ask questions.
- GLASSES: You can choose to have a monofocal (single focus) IOL implanted for distance vision and wear separate reading glasses, or have the IOL implanted for near vision and wear separate glasses for distance.
- MONOVISION: The ophthalmologist could implant IOLs with two different powers, one for near vision in one eye, and one for distance vision in the other eye. This combination of a distance eye and a reading eye is called monovision. It can allow you to read without glasses. Many patients who wear contacts or who have had refractive surgery have monovision and are happy with it. Your surgeon will discuss and demonstrate this option to see if it might work for you. However, unless you have previous experience with monovision contact lenses, your surgeon will probably not recommend this option.
- MULTIFOCAL IOL: The ophthalmologist could implant a “multifocal” IOL. This is a newer, “premium” type of IOL that provides distance vision AND restores some or all of your eye’s ability to focus at other ranges, such as near or intermediate. Choosing this option will usually lead to higher out-of-pocket expenses since most insurance companies only pay for a monofocal (single focus) lens. However, if this option is of interest to you and you are determined to be an optimal candidate by the Doctor, there are payment plans available to overcome the financial barriers in making this choice.
Information about treating astigmatism
Patients with nearsightedness and farsightedness often also have astigmatism. An astigmatism is caused by an irregularly shaped cornea; instead of being round like a basketball, the cornea is shaped like a football. This change in shape can make your vision blurry. There are several treatment options for astigmatism: 1) you can have an IOL for near or distance vision and continue to wear glasses or contact lens for the astigmatism; 2) you can have a Toric IOL placed in your eye, 3) you can have refractive surgery called LASIK or PRK, or 4) your surgeon can perform a procedure before, during, or after cataract surgery called a limbal relaxing incision. A limbal relaxing incision (LRI) is a pair of small, precise incisions the ophthalmologist makes into your cornea to make its shape rounder. Enhancement incisions may be required in order to achieve optimal results.
ANESTHESIA
The ophthalmologist and the nurse anesthetist will anesthetize your eye with topical anesthesia. You may also undergo light sedation administered by a nurse anesthetist, or elect to have the surgery with topical anesthesia only. The risks associated with anesthesia and sedation are addressed under the Risks of Cataract Surgery section of this packet and will be discussed with you individually by your ophthalmologist and nurse anesthetist.
PROCEDURE
An incision, or opening, is made in the eye. This is at times self-sealing but it may require closure with very fine stitches which will gradually dissolve over time. The natural lens in your eye will then be removed. There are several ways to remove the lens; the most common technique is called phacoemulsification, which uses a vibrating probe to break the lens up into small pieces. These pieces are gently suctioned out of your eye through a small, hollow tube inserted through a small incision into your eye. After your natural lens is removed, the IOL is placed inside your eye. In rare cases, it may not be possible to implant the IOL you have chosen or any IOL at all.
POSTOPERATIVE CARE
Your eye will be examined the day after surgery by your surgeon or an eye doctor chosen by your surgeon, and then at intervals determined by your surgeon. During the immediate recovery period, you will place drops in your eyes for 2 to 4 weeks. If you have chosen monovision or a multifocal IOL to reduce your dependency on glasses or contacts, they may still be required either for further improvement in your distance vision, reading vision, or both. You should be able to resume your normal activities within 2 or 3 days, and your eye will usually be stable within 1 to 3 weeks, at which time glasses or contact lenses could be prescribed.
AFTER CATARACT SURGERY
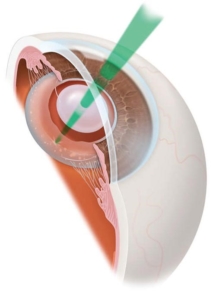 Regardless of the type of IOL chosen, you may need laser surgery (a YAG capsulotomy) to correct clouding of the capsule that holds the intraocular lens in place. This occurs in up to 1 in 5 patients after cataract surgery and is easily correctable with the laser.
Regardless of the type of IOL chosen, you may need laser surgery (a YAG capsulotomy) to correct clouding of the capsule that holds the intraocular lens in place. This occurs in up to 1 in 5 patients after cataract surgery and is easily correctable with the laser.
After your cataract surgery the back membrane of the cataract which is left in place to support the lens implant may become cloudy and cause blurred vision. Sometimes patients will see streaks or halos around lights.
In the past, a trip back to the operating room was necessary. Fortunately, a modern YAG laser treatment can be performed without a need for an anesthetic injection or a small cut. The laser utilizes a narrow wavelength of light to disrupt the opacification on the lens capsule. There is no pain, no interruption in physical activities and no patch is required after the laser treatment.
Cataract Patients See Improved OutcomesWith Breakthrough ‘Intraoperative’ ORA Technology
For the first time in medical history, cataract surgeons have the on-demand ability to measure outcomes, correct astigmatism and verify lens implant calculations in real time during cataract surgery… Click Here to read the article!

